Polio Place
A service of Post-Polio Health International
High Tech Breathing
Category: Essays
David Cotcher
Breathing is fundamental to life. If we do not take in sufficient oxygen or get rid of carbon dioxide (CO2) it affects every part of our body. I had polio at about 18 months and at seven I started to have a curvature of my back that developed into a double curvature called kyphoscoliosis. As I grew my muscles were weaker on one side than the other causing my back and rib cage curvature. This restricts my lung volume.
Muscle weakness also affects my breathing. The problem is worsened when lying down and I was not breathing deeply enough when sleeping. I was prescribed supplementary oxygen usage starting in 1995 after I had pneumonia. This allows me to get sufficient oxygen with less effort, but this can compound the problem of my lungs not getting rid of the CO2 build up in my blood. More about the effects I had from polio are told in "My Polio Story" in the May 2009 issue of Polio PostBox (newsletter of Polio Regina, Saskatchewan).
In 2007 I ended up in hospital about 10 days in January, another 10 days in early February with worsening respiratory condition, and then back in hospital with respiratory failure from high CO2 in my blood later in February. I was in critical condition with my oxygen level down to 31% and my CO2 level 3 to 4 times the limit. High CO2 leads to being incoherent, then unconscious, and then to death. I had been getting more incoherent over the previous weeks and was slipping into unconsciousness. I ended up with a tracheostomy and on a respiratory ventilator to help keep my CO2 level under control. I was there recovering until mid-April. I improved quite well and was able to go back to work part time by June. I still have a trach and use the ventilator at night to improve my breathing while I sleep. Follow up tests show that my CO2 level is still under control.
For this reason I have continued using a respiratory ventilator at night to keep a proper balance of oxygen and CO2 in my system. I used a BIPAP (Bi-level Positive Airway Pressure) machine for a while in January/ February 2007 but my condition continued to worsen and I need the extra support of a volume ventilator. The ventilator I used for 5 years is called a Phillips Respironics PLV 100. It is called a volume ventilator because it gives a measured volume of air on each breath. At night it is connected through a hose to my trach tube. It is set to give me 0.37 liters of air on each breath for a minimum of 10 breaths per minute. Room air is about 21% oxygen, but extra oxygen is added to the ventilator air to bring it up to 30%.
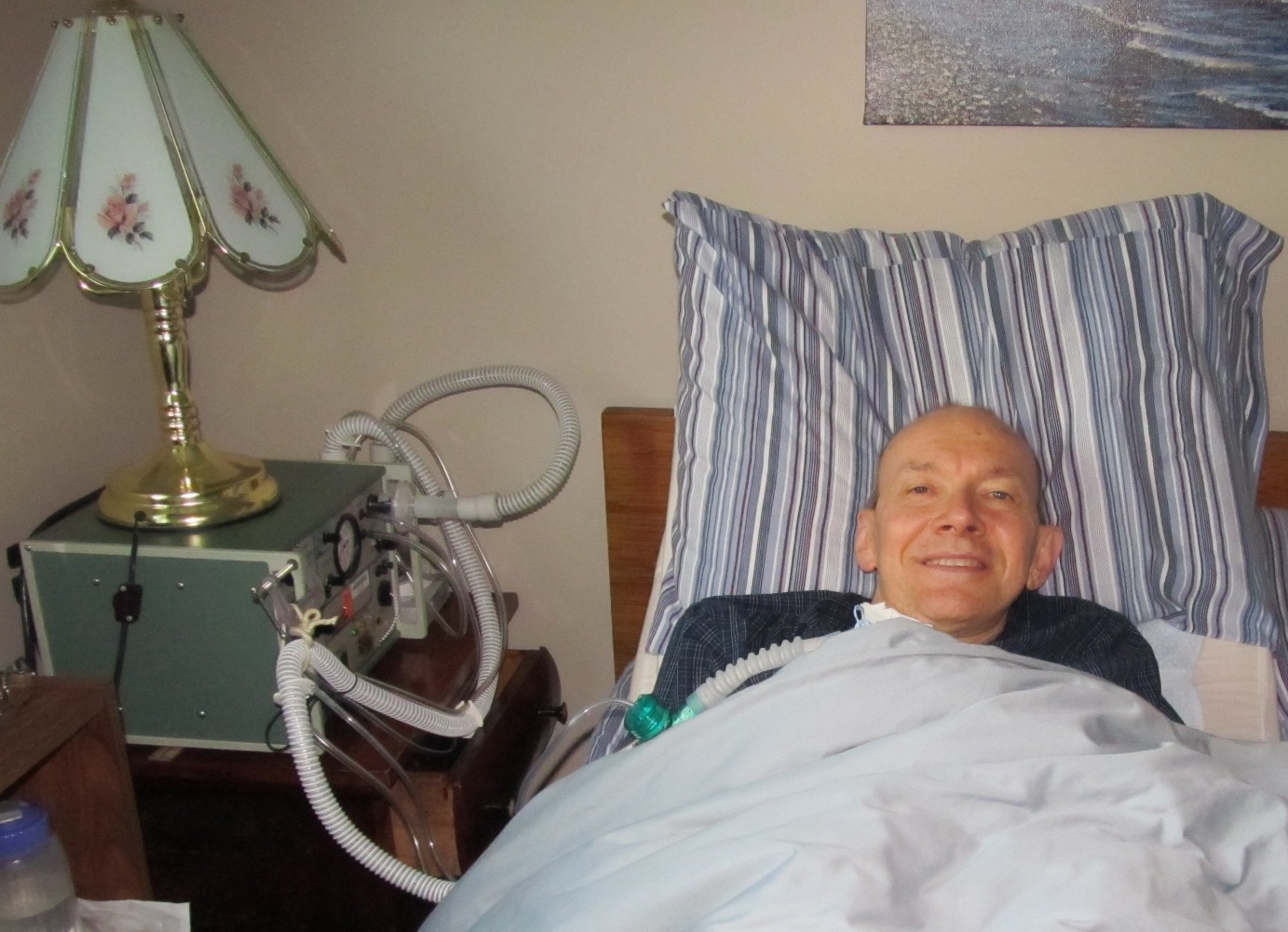 The first picture shows with me in bed connected to the old PLV 100 ventilator. The ventilator is on a bed side table (with a lamp sitting on top of the ventilator) as seen in the picture. I used this same model of ventilator each night for five years starting when I was in the hospital in 2007. The PLV 100 ventilator model is out of date and no longer supported by the manufacturer. It is a simple and reliable machine, sometimes with a few clunks, honks and rattles, but it just keeps puffing along. The family says I sounded like a steam engine when using it. It is a pretty rugged machine and I told the respiratory therapist it looks like it was designed to mount in the back of an army truck.
The first picture shows with me in bed connected to the old PLV 100 ventilator. The ventilator is on a bed side table (with a lamp sitting on top of the ventilator) as seen in the picture. I used this same model of ventilator each night for five years starting when I was in the hospital in 2007. The PLV 100 ventilator model is out of date and no longer supported by the manufacturer. It is a simple and reliable machine, sometimes with a few clunks, honks and rattles, but it just keeps puffing along. The family says I sounded like a steam engine when using it. It is a pretty rugged machine and I told the respiratory therapist it looks like it was designed to mount in the back of an army truck.
Then earlier this year we got the news that the provincial health department had approved the purchase of new ventilators. The respiratory therapist brought mine in mid-May to get me going using it. The new machine is a Covidien Puritan Bennett 560 ventilator* which is the latest technology. The second picture shows me in bed connected to the new PB 560 ventilator. The heated humidifier behind the ventilator is the same one I used with the old machine.
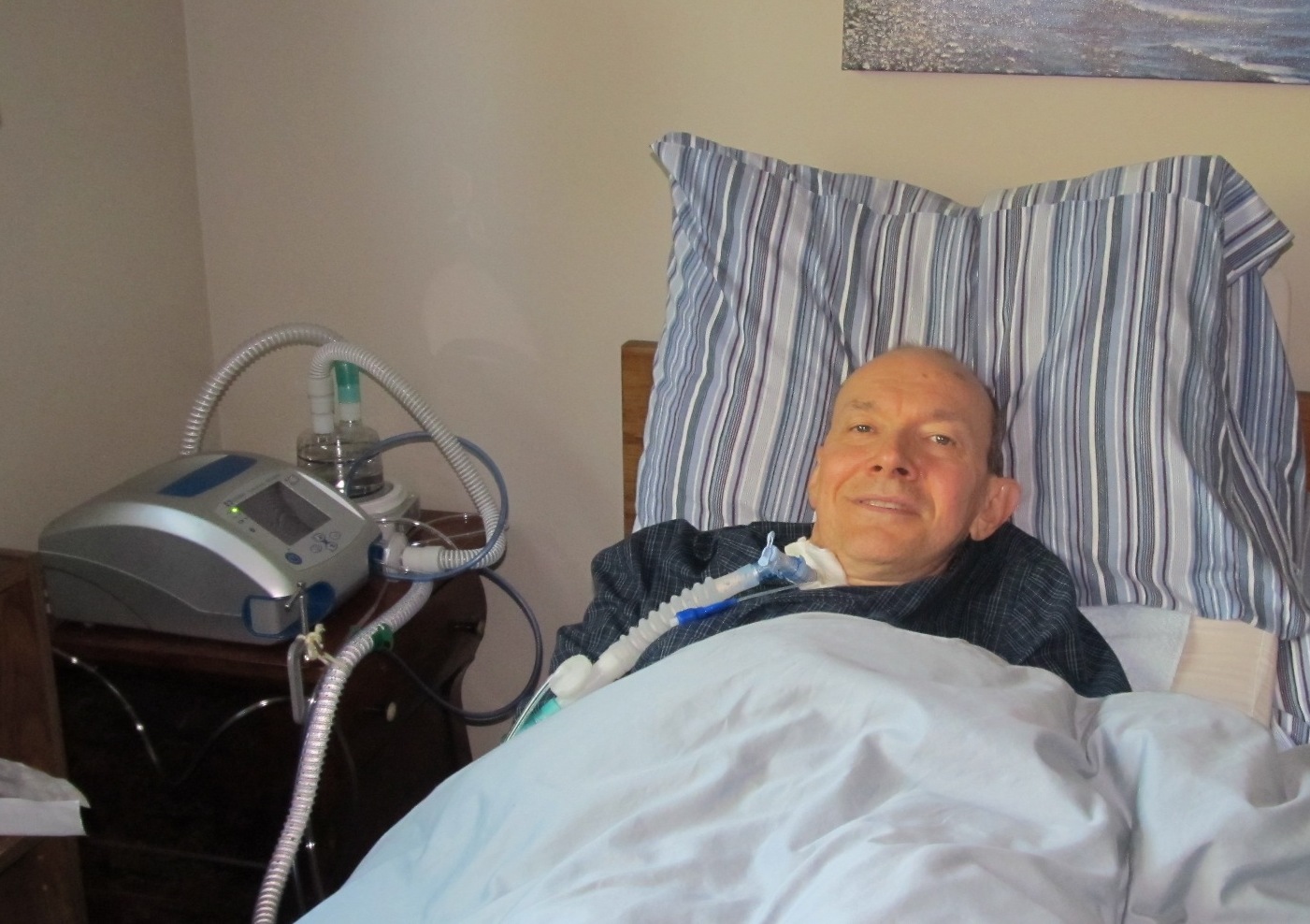 When I used the new ventilator for the first night, I woke up after sleeping one hour and then had some trouble getting used to it before sleeping and waking several more times. After being used to the feel and sound of the old machine it takes some getting used to sleeping with the new one. The old ventilator we called a "steam engine" with the sound of a large piston cycling back and forth with each breath. The new machine has a variable speed micro turbine (like a tiny "jet engine") that has a varying higher pitched whirring sound with each breath. The feel of the breathing cycle is different as well. The following nights were still more difficult sleeping and I would wake feeling like I was not getting my breath. But night by night there was some improvement in being more relaxed and comfortable to sleep with the new ventilator. Now I have been using the new ventilator for about 5 months and I am getting used to sleeping with it, although it still takes a little while at the start of each night to relax and not think about the sound or feel of the machine.
When I used the new ventilator for the first night, I woke up after sleeping one hour and then had some trouble getting used to it before sleeping and waking several more times. After being used to the feel and sound of the old machine it takes some getting used to sleeping with the new one. The old ventilator we called a "steam engine" with the sound of a large piston cycling back and forth with each breath. The new machine has a variable speed micro turbine (like a tiny "jet engine") that has a varying higher pitched whirring sound with each breath. The feel of the breathing cycle is different as well. The following nights were still more difficult sleeping and I would wake feeling like I was not getting my breath. But night by night there was some improvement in being more relaxed and comfortable to sleep with the new ventilator. Now I have been using the new ventilator for about 5 months and I am getting used to sleeping with it, although it still takes a little while at the start of each night to relax and not think about the sound or feel of the machine.
One big advantage of the new ventilator is that it is much lighter to take with us when we travel. It just has a zippered soft case with a shoulder strap for carrying. The old one had a large heavy steel framed shipping case. The PLV 100 machine weighed 12.8 kg (28 lb) and over 18 kg (40 lb) with the shipping case. The new PB 560 ventilator is only 4.5 kg (11 lb) with a light carrying case. Not having to take the old heavy ventilator in and out when we travel made my wife Elaine very happy. We did try out traveling with the new ventilator when we went away for some weekends as well as a 10 day trip and all went well.
It took some time to get used to my new ventilator. But I am thankful I can sleep comfortably at night now with my "hi tech" breathing assistance.
*see Home Ventilator Guide for details.
Tagged as: breathing