Polio Place
A service of Post-Polio Health International
Essays
Index
Lawrence C. Becker
Nancy Baldwin Carter
David Cotcher
Richard Lloyd Daggett
Anne K. Gross, PhD
Lauro S. Halstead, MD
Ernest W. Johnson, MD
Kathleen A. Navarre
Sunny Roller
Fr. Robert J. Ronald, SJ
Linda Cannon Rowan
William Stothers
Grace Young
STILL HERE, AFTER ALL THESE YEARS
 Lawrence C. Becker
Lawrence C. Becker
“You had polio? I thought they cured that."
If I had $10 for every time I’ve heard those words, I could sponsor a vaccination program in a village in some hard-to-reach part of the world. That would be a good thing. But polio is not “cured” by the vaccines—it is prevented. There’s a difference.
Polio is not over. There are millions of survivors. Some of us are living with a substantial physical disability and have had rewarding family lives and productive careers in fields where we never have to mention or even think about polio. Some have a weak leg, or a weak voice, or a shoulder that dislocates every now and then, but have almost forgotten about the cause. And some don’t have the luxury of forgetting about polio even for a day – either because the initial disability was overwhelming, or because the surprising second punch of the disease (post-polio syndrome, which occurs decades after the initial infection) is devastating, or because they devote their working lives to rehabilitation medicine, or health policy, or assistive services.
We’re all still here -- for the duration of an average lifespan, apparently. In the US alone, there are three quarters of a million polio survivors still standing (or sitting). We have some things to bring to your attention this week.
We think there are still good lessons to be learned from polio – lessons about diseases, injuries, disabilities and epidemics of many sorts. The polio epidemics are over in the United States, and in most places throughout the world. The eradication effort continues, and must be brought to a successful conclusion. But the persistence, and courage, and genius that brought us the vaccines in the 1950s is not the only important thing to remember from the polio years.
At the top of my list of things to remember, for example, is “functional” rehabilitation. This is the part of rehabilitation that goes on after you are out of danger medically, and after the extent of your permanent disability is known, and after you’ve gotten all that shiny new equipment – wheelchair, or braces, or other assistive devices. What remains after all of that is the job of making it work; making it truly functional. This takes time, effort, and resources.
For example, when it became clear to everyone around me, in early 1953, that my hands and arms were never going to be usable again, the occupational therapists in the rehab hospital taught me how to do some unusual things with my feet – writing, for one, and typing. Those things became very useful, eventually. But the OTs, for their own therapeutic reasons, also taught me how to do all sorts of things with my feet, or with a mouthstick: to draw, to weave a scarf on a small loom, to move chess pieces around on a chessboard, and other things. All of them were exhausting. Some of them were actually dangerous. (Ever try to use a wood burning craft kit with your feet? In a hospital bed? The former Cub Scout in me insisted on it, against the OT’s better judgment.) Most of these things I didn’t do very well, and didn’t want to do at all. My mother was delighted with the scarf, but I don’t think she actually ever wore it in public! And the writing and typing, which I did very much want to do, didn’t become genuinely functional skills for several years. It took a long time, and it was hard work.
I raise this issue only because I am worried about rehabilitation practices today – rehabilitation for spinal cord injuries, stroke, and traumatic brain injury, for example. It seems to me that people are getting shortchanged with respect to long-term, functional rehabilitation. I’ve seen this in the research projects I’ve helped monitor at the National Institutes of Health; I’ve seen it in the appalling news reports about the lack of long-term rehabilitation given to badly injured veterans of the Iraq war (especially those with traumatic brain injuries); and I’ve seen it in the crowded physical and occupational therapy units here in Roanoke, where therapists are required by the limitations of insurance coverage to try to compress their outpatient work into a few weeks of sporadic visits.
When I raise this issue with physicians, researchers, therapists, and even patients, I quickly hit a stone wall. I compare today’s “brief therapy” to the extraordinary length of my own inpatient rehabilitation (2 ½ years), or to the length of time it took Franklin Delano Roosevelt to get to the place that allowed him to resume his political career. Often, I get an answer that is too much like remarks about polio’s being cured, or its being over.
People say, “Things are different now. The technology is so much better. The hospital stays are shorter. There are fewer social and legal barriers for disabled people. There are curb cuts, and ramps, and automatic doors, and accessible bathrooms in public places everywhere. We see people motoring around in wheelchairs or on scooters in malls. Life is faster, and more expensive. Rehabilitation is faster, and more expensive. And better, no? ”
Not so much. All of that misses my point. Some things just take time and effort, not more and more expensive technology. Three to six months of hospitalization and intensive therapy is now typically the outside limit for even the most severe injuries. Modern medicine is good, but it’s not that good.
If I had been discharged after six months, I would have been a quadriplegic in an iron lung. I wouldn’t have had any genuine functional therapy at all by that time, and I probably wouldn’t ever have gotten any because merely caring for me at home – keeping me alive and reasonably comfortable -- would have been a consuming project for my family. Getting access to functional therapy would have been so exhausting for everyone that it would have been demoted to a low priority.
Yes, things are better now, but in the functional therapy line, mostly they’re just more expensive. The body still takes its own good time to heal. People have limited energy – not to mention limited patience for weaving ugly scarves in unusual ways -- even if it helps develop the muscles needed for genuinely functional skills. If getting yourself dressed in the morning takes two hours, after which you have to rest for two more, dressing yourself is not yet a functional skill. Loving families are typically too ready to say “Here, let me help you with that.” There is no substitute for relentless, inventive, no-nonsense, long-term functional therapy, guided by unsentimental professionals.
Polio survivors in the United States had this – at least throughout and after the epidemics in the late 1940s and 1950s. We’ve done well all these years because of it. Physiatrists, physical therapists, orthotists, occupational therapists were available to us for extended periods of time, and we still go back for regular tune-ups. It is a lifelong effort. We just don’t talk about it very much.
It would be a shame if people forgot this lesson from the polio epidemics. So the next time you read about traumatic brain injury, pay attention to the part about rehabilitation – how long it takes, whether people are getting enough of it.
The next time you read about someone with an injury like Christopher Reeve’s, but without his financial resources, being discharged to a nursing home after three months in a hospital, pay attention to what is said (if anything) about plans for functional rehabilitation.
Don’t be dazzled by accounts of all the fancy, expensive equipment supplied to these folks. Unless we actually stick with them long enough for them to acquire genuinely functional abilities, all they (and we) will get from all that equipment is a few badly made scarves that only a mother could love.
A much better way has already been pioneered. Let’s remember it.
Lawrence C. Becker is a retired philosophy professor, who had polio at the age of 13, in 1952.
POLIO AND ME: AN INSIDE LOOK
Nancy Baldwin Carter
One day I was running wild through the exhibits at the Thayer County Fair in Nebraska, a typical eleven-year-old shrieking uncontrollably as the Octopus ride tossed me hither and yon, winning a kewpie doll pitching plastic balls through embroidery hoops. The next, I was in bed with the “flu,” soon to be rushed to the hospital a hundred miles away, cradled in my mother’s arms in the back seat of the car, struggling for breath. That’s the way it was in August 1948.
Someone deposited me into the polio isolation unit and left me there. Alone in a large, dark room, I was having trouble breathing. I discovered I could not move any part of my body, and in an attempt to cry for help, I learned my voice box didn’t work, either. I could not utter a sound. I was terrified. I listened to the wail of ambulances through the open hospital window near my bed, and soon I lost consciousness.
By the next August I had spent five months in the hospital, then seven at Warm Springs, had gone through all the therapies, been braced to the hilt, and was ready to rise from my wheelchair and dive back into life. It took another eight years to train my body to function without the brace—and until today to fully understand what I had gone through.
Life did go on. And I did all the stuff. Or nearly all of it. I went to school and ended with a masters degree. I began professionally as a high school English teacher and ended as an adult education administrator. I made friends, developed relationships, and ended with a super-boffo husband.
When post-polio issues entered the picture, I began working for the cause. I jumped into creating a state-wide polio survivor association that clicked. We were all caught up in a swirl of meaningful activity, carrying the message to thousands, shining light in the darkest corners. By the time I had to step down, I knew that Post-Polio Syndrome finally had me literally by the throat. Once again paralyzed, I started over, this time with extensive surgery, then bracing, a power chair, and using the ventilator.
It’s always hard to admit there are things I cannot do anymore. I don’t relish facing such changes. But I remember the “you’ll have to want what you have, not have what you want” admonition someone lectured me with years ago. As I age and my wasted body shrinks itself like a plum on its inevitable journey to prunedom, I recognize that more and more is quite truly out of my reach.
At first I had to move freely, as “normal” people do. I had worked so hard to get rid of my body/head brace in my college days; the last thing on earth I wanted was to start wearing one again. And I hoped never to possess another wheelchair. So I refused to wear the new brace and fooled around with a manual chair I couldn’t operate. I was miserable. Finally I had to face reality: I will never again be that other person, the one who walks two miles on the jogging path every day, who jumps into the car after a loaf of bread at the market, who pops in to see a friend and take her out to lunch. Perhaps I never was, I’m not sure. What I am sure of is that from the moment I sat in my new power chair with its unexpectedly magic joy stick, I had what I had longed for. I was lifted from the bonds of a stubbornly useless body by an ill-fitting brace and an unwieldy, jet-black chair. I am free. I can move. I can fly down the winding path next to the swans in the lagoon and bustle my way from store to store among the shoppers at the mall. I love it. And when the time comes for me to admit, “I cannot do this anymore” once again—well, I’ll deal with that when it happens. I’m doing this today, and today is what I have.
Polio left me with a lot of advantages. I learned not only to be independent, but to insist on it. I know what it takes to stand fast against the storm. I’m ready to fight for me.
I’ve had the best teachers—wonderful polio doctors, for example, who showed me the value of a hearty laugh and proved that we humans can be brilliant and compassionate at the same time. And all the while, showering me with words of independence.
But perhaps the most significant thing I’ve learned is a gift that came to me by chance. Pure luck. In 1984 I had returned to Warm Springs for a diagnosis of PPS. An exceptional doctor there spent a great deal of time with me, explaining my condition and educating me in the ways of post polio. Five years later, the overused muscles in my upper body gave out. I could not sit up or feed myself or control the movement of my head. There seemed to be no way out. I was scared to death. An orthopedist came to the house to examine me, and then a neurologist. Both said they could do nothing to help. I felt abandoned, drowning in despondency.
Then I remembered the Warm Springs doctor. I got her on the telephone and tearfully explained my situation. She spoke with me for a long time that day, and finally I heard her say in that soft, sweet Georgia accent of hers, “Accept it, Nancy.”
Suddenly a weight was lifted from that miserable body of mine. I was at peace. It was a powerful moment, a lesson I hope never to forget. All I have to do is be willing to accept my circumstances, and I get to feel serene and happy. The mind trumps the body. Even today when this body malfunctions, as it does far too often, I try to summon the willingness to “accept it.” This is never easy, but it is always the solution.
My ace in the hole is my husband. He indulges me. Pampers me. Laughs with me. Whatever I need, he’s here to help. He has rushed me to the emergency room; he has fed me when I can’t raise an arm. He bathes me, empties my commode, takes me out into the sunshine. Yet, it’s so much more than that. He loves me. Just as I am. And even though I’m not the, uh, ravishing beauty he married, this little particular doesn’t seem to matter; he sees the me inside. It’s not simply that he arranges the pillows that ease my pain; it’s that he arranges the pillows. And the task is done with sweetness, compassion, and genuine care. Who would I be without this amazing presence in my life? Would I be at all? I wonder. This is a very special man.
There seems to be no adequate way to paint the picture I’m attempting to. I’m shocked that, in order to describe how I handle aging, I want to talk about the toll taken when age and PPS conspire against me. I think of railing against the fates, of devising ways to triumph over the odds. Details, mere facts. Not the way I feel. In truth, my life is much simpler than that. I wake up in the morning. I do what I can. I deal with today. If I’m still here by bedtime, it’s been a good day. I am happy.
There’s a spiritual aspect to all of this that I don’t totally understand. I’m aware today as I never was before that I don’t get to have my way all the time and, significantly, this is a good thing. I don’t have God’s vision. I can’t begin to predict the ramifications of my will. I can’t see down the path; I don’t always know what’s best. As a result, I try to give up my headstrong mulishness and merely let the day happen. In many ways, it’s a relief not to have to shoulder the burden of my capricious life. I mean to open myself to the possibilities, to step back and allow the future to unfold.
Yet, I cannot lie. Sometimes I can’t stop fighting, and occasionally fear gnaws at the corners of my being. There are days when darkness enfolds me and I am alone in the certainty of this disability. For a moment I am lost in despair. Then I remember the hope of tomorrow. If I can get through today, I tell myself, by tomorrow the pain may be gone. It could happen, I say. It could happen. And frequently it does. It’s no longer in my hands. Even so, and perhaps this surprises even me, I like where I am and who I am. Maybe that’s the key. Yeah, I’m OK today.
Nancy Baldwin Carter, B.A, M.Ed.Psych, from Omaha, Nebraska, is a polio survivor, a writer, and is founder and former director of Nebraska Polio Survivors Association.
High Tech Breathing
David Cotcher
Breathing is fundamental to life. If we do not take in sufficient oxygen or get rid of carbon dioxide (CO2) it affects every part of our body. I had polio at about 18 months and at seven I started to have a curvature of my back that developed into a double curvature called kyphoscoliosis. As I grew my muscles were weaker on one side than the other causing my back and rib cage curvature. This restricts my lung volume. Muscle weakness also affects my breathing. The problem is worsened when lying down and I was not breathing deeply enough when sleeping. I was prescribed supplementary oxygen usage starting in 1995 after I had pneumonia. This allows me to get sufficient oxygen with less effort, but this can compound the problem of my lungs not getting rid of the CO2 build up in my blood. More about the effects I had from polio are told in "My Polio Story" in the May 2009 issue of Polio PostBox (newsletter of Polio Regina, Saskatchewan).
In 2007 I ended up in hospital about 10 days in January, another 10 days in early February with worsening respiratory condition, and then back in hospital with respiratory failure from high CO2 in my blood later in February. I was in critical condition with my oxygen level down to 31% and my CO2 level 3 to 4 times the limit. High CO2 leads to being incoherent, then unconscious, and then to death. I had been getting more incoherent over the previous weeks and was slipping into unconsciousness. I ended up with a tracheostomy and on a respiratory ventilator to help keep my CO2 level under control. I was there recovering until mid-April. I improved quite well and was able to go back to work part time by June. I still have a trach and use the ventilator at night to improve my breathing while I sleep. Follow up tests show that my CO2 level is still under control.
For this reason I have continued using a respiratory ventilator at night to keep a proper balance of oxygen and CO2 in my system. I used a BIPAP (Bi-level Positive Airway Pressure) machine for a while in January/ February 2007 but my condition continued to worsen and I need the extra support of a volume ventilator. The ventilator I used for 5 years is called a Phillips Respironics PLV 100. It is called a volume ventilator because it gives a measured volume of air on each breath. At night it is connected through a hose to my trach tube. It is set to give me 0.37 liters of air on each breath for a minimum of 10 breaths per minute. Room air is about 21% oxygen, but extra oxygen is added to the ventilator air to bring it up to 30%.
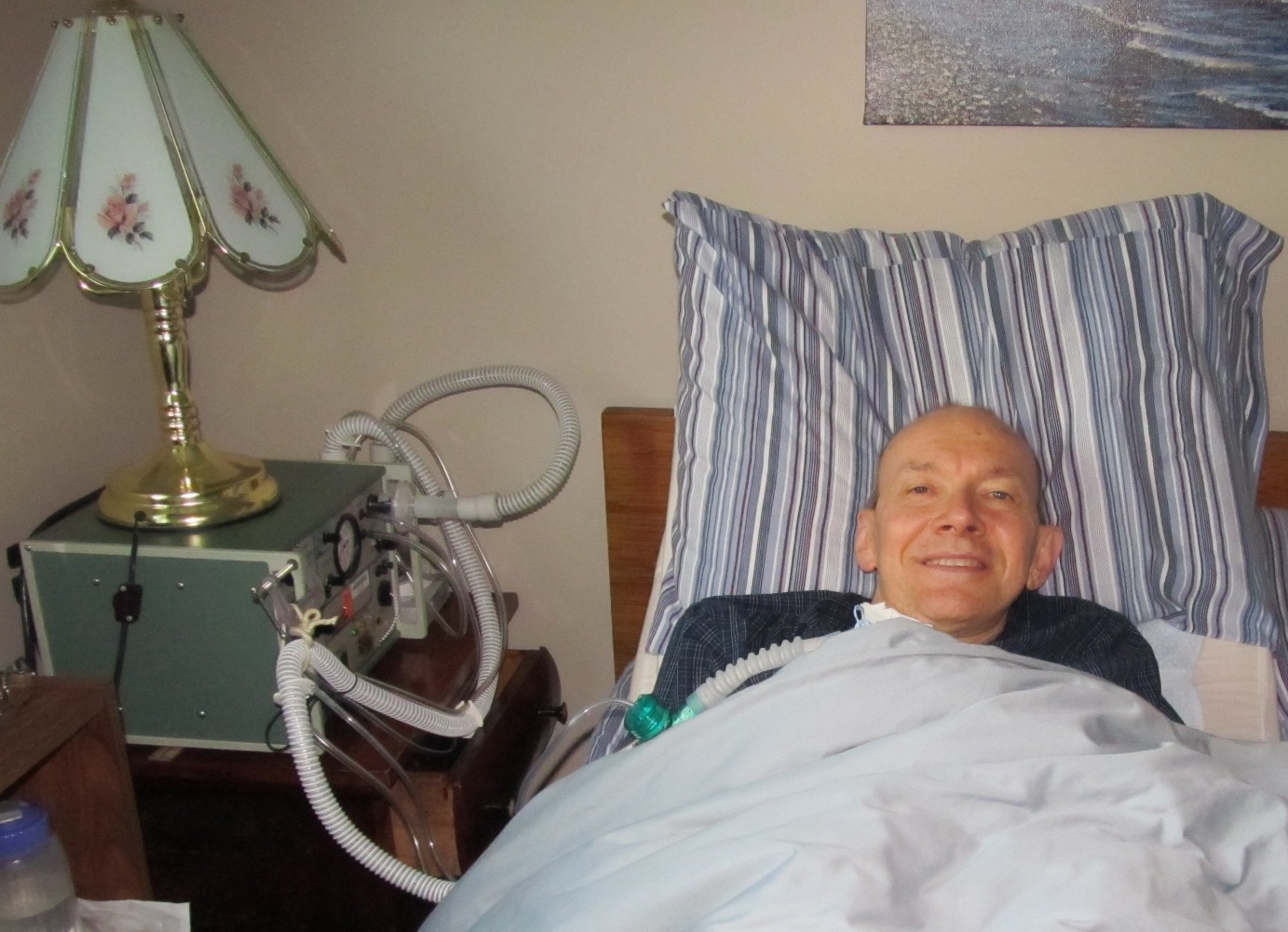 The first picture shows with me in bed connected to the old PLV 100 ventilator. The ventilator is on a bed side table (with a lamp sitting on top of the ventilator) as seen in the picture. I used this same model of ventilator each night for five years starting when I was in the hospital in 2007. The PLV 100 ventilator model is out of date and no longer supported by the manufacturer. It is a simple and reliable machine, sometimes with a few clunks, honks and rattles, but it just keeps puffing along. The family says I sounded like a steam engine when using it. It is a pretty rugged machine and I told the respiratory therapist it looks like it was designed to mount in the back of an army truck.
The first picture shows with me in bed connected to the old PLV 100 ventilator. The ventilator is on a bed side table (with a lamp sitting on top of the ventilator) as seen in the picture. I used this same model of ventilator each night for five years starting when I was in the hospital in 2007. The PLV 100 ventilator model is out of date and no longer supported by the manufacturer. It is a simple and reliable machine, sometimes with a few clunks, honks and rattles, but it just keeps puffing along. The family says I sounded like a steam engine when using it. It is a pretty rugged machine and I told the respiratory therapist it looks like it was designed to mount in the back of an army truck.
Then earlier this year we got the news that the provincial health department had approved the purchase of new ventilators. The respiratory therapist brought mine in mid-May to get me going using it. The new machine is a Covidien Puritan Bennett 560 ventilator* which is the latest technology. The second picture shows me in bed connected to the new PB 560 ventilator. The heated humidifier behind the ventilator is the same one I used with the old machine.
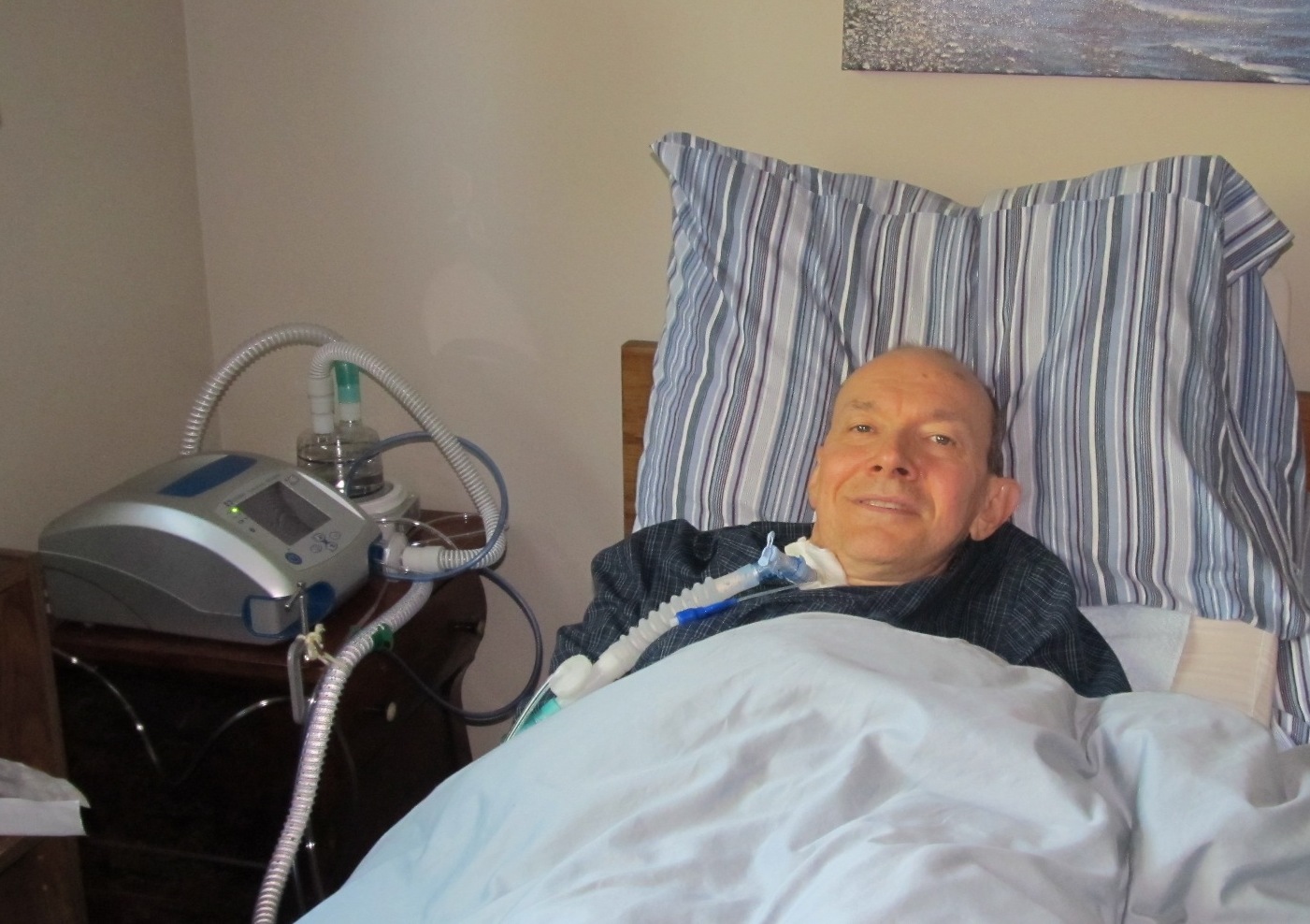 When I used the new ventilator for the first night, I woke up after sleeping one hour and then had some trouble getting used to it before sleeping and waking several more times. After being used to the feel and sound of the old machine it takes some getting used to sleeping with the new one. The old ventilator we called a "steam engine" with the sound of a large piston cycling back and forth with each breath. The new machine has a variable speed micro turbine (like a tiny "jet engine") that has a varying higher pitched whirring sound with each breath. The feel of the breathing cycle is different as well. The following nights were still more difficult sleeping and I would wake feeling like I was not getting my breath. But night by night there was some improvement in being more relaxed and comfortable to sleep with the new ventilator. Now I have been using the new ventilator for about 5 months and I am getting used to sleeping with it, although it still takes a little while at the start of each night to relax and not think about the sound or feel of the machine.
When I used the new ventilator for the first night, I woke up after sleeping one hour and then had some trouble getting used to it before sleeping and waking several more times. After being used to the feel and sound of the old machine it takes some getting used to sleeping with the new one. The old ventilator we called a "steam engine" with the sound of a large piston cycling back and forth with each breath. The new machine has a variable speed micro turbine (like a tiny "jet engine") that has a varying higher pitched whirring sound with each breath. The feel of the breathing cycle is different as well. The following nights were still more difficult sleeping and I would wake feeling like I was not getting my breath. But night by night there was some improvement in being more relaxed and comfortable to sleep with the new ventilator. Now I have been using the new ventilator for about 5 months and I am getting used to sleeping with it, although it still takes a little while at the start of each night to relax and not think about the sound or feel of the machine.
One big advantage of the new ventilator is that it is much lighter to take with us when we travel. It just has a zippered soft case with a shoulder strap for carrying. The old one had a large heavy steel framed shipping case. The PLV 100 machine weighed 12.8 kg (28 lb) and over 18 kg (40 lb) with the shipping case. The new PB 560 ventilator is only 4.5 kg (11 lb) with a light carrying case. Not having to take the old heavy ventilator in and out when we travel made my wife Elaine very happy. We did try out traveling with the new ventilator when we went away for some weekends as well as a 10 day trip and all went well.
It took some time to get used to my new ventilator. But I am thankful I can sleep comfortably at night now with my "hi tech" breathing assistance.
*see Home Ventilator Guide for details.
NOT JUST POLIO: MY LIFE STORY
Excerpts from the autobiography (Not Just Polio: My Life Story) of Richard Lloyd Daggett, polio survivor and ventilator user:
July, 1953
My mother drove to the hospital to visit almost every afternoon and both parents came in the evening. I’m sure it was a difficult time for them. I was their youngest child, and I was very, very ill with bulbospinal polio, the most severe form of this disease. I learned later that, in addition to polio, I had a life-threatening case of pneumonia.
It was probably more difficult for all the parents. Imagine entering a room filled with these huge metal tanks. The tanks are making their whooshing sound. All you can see are heads sticking out one end of each tank, and you know that one of these heads belongs to your child.
My father began a daily journal of the events surrounding my illness and hospitalization. He never mentioned it, and I didn’t know about it until after his death when I was going through his papers. I believe this journal was his way of coping with the strain and sadness he and my mother must have endured.
Here are some excerpts from the first few entries:
Friday, July 17: Dr. Hershey examined him and gave us an order to take him to the CD building at the General Hospital. Arrived about 11:30 a.m. They asked us a lot of questions and gave Richard an examination. He said he felt “Pretty good,” The doctor told us he had no muscular weakness at that time.
Saturday, July 18: Arrived at the hospital at 2 p.m. Richard was suffering some discomfort and said, “I have it”, meaning polio. He showed us the difficulty he had moving his arms. We returned home somewhat apprehensive. At 9 p.m. Dr. Miller called and said Richard developed some difficulty breathing and they were planning to put him in an Iron Lung later in the evening. He called again about 11:30 and suggested we come there. We went immediately. We couldn’t see the doctor until 2:15 a.m. He explained they put Richard in the Lung as a precaution and to save his strength. We went home feeling pretty low.
Sunday, July 19: Called the hospital at 9 a.m. The nurse said Richard had a quiet night and that we could see him. We went right over and visited with him for 10 minutes. He seemed in good spirits, under the circumstances, and was comfortable. Talked to one of the Drs. and he explained some things about polio to us. As long as the patient has a fever it is still “working”. After that they can determine the extent of nerve damage. There is nothing to do but wait for two or three days for the answer. They will be anxious days for us. Went to the hospital again in the evening. Richard is a very sick boy.
Monday, July 20: I left work at noon. Went home for lunch and we went to the hospital. The nurse was working on Richard when we saw him. The Dr. said he had developed pneumonia. Still a very sick boy. We returned to the hospital at 7 p.m.. We were rewarded with the first hopeful sign. Richard seemed in good spirits and the nurse said his temperature was down a little. We came home clinging to that slim thread of hope.
Tuesday, July 21: Came home for lunch and went to the hospital. The nurse was working on Richard so we had to wait in the hall a few minutes before we could see him. He is very sick but the Dr. said his fever is slightly lower. He also told us that Richard has a better than even chance to pull through. Returned to the hospital at 7 p.m. Richard was asleep when we went in but the nurse awakened him. He seemed glad to see us. I asked him if he was discouraged and he shook his head to indicate a definite “NO!” That spirit can’t lose and I’m real sure he will win.
I treasure this journal. It is important historically, but even more important to me is the written record of my parents’ thoughts and concerns.
Summing Up
Through all the twists and turns my life has taken, whether public or private, I’ve had the support of my family. My parents always encouraged me in whatever tasks I undertook. Living with them was certainly to my advantage. Not just because they could provide the assistance I needed in daily activities, but because we enjoyed doing so many things together. I know I would not have traveled as much, nor had as wide a spectrum of experiences, if it were not for them. I’ve also had the support of my brothers and sister and the encouragement of many friends. In this respect, I have been blessed.
My parents were also responsible for how I dealt with polio. I never heard them say, “Poor Richard,” or any other expressions of pity. My father had a positive, no-nonsense attitude. His advice equated to, “OK, You hit a pothole. Now move on.” He would sometimes say to me, “Don’t say ‘I can’t do this.’ Say you’re having difficulty.” My mother was a little more protective. After all, she was my mother. But even she expected that I live my life positively.
I have been so fortunate. Yes, I had polio, but I contracted this disease in Los Angeles County. The county had the resources to give the best medical care possible. With additional funding from the March of Dimes, the county built Rancho Los Amigos, the largest and most up-to-date treatment facility for respiratory polio patients in the nation. Rancho gave me the finest rehabilitation available and continues to monitor my pulmonary health. I doubt I would be alive today if it weren’t for Rancho’s timely medical interventions.
I was asked once by a television reporter what I thought my life would have been like had I not contracted polio. I replied that people can’t, or at least shouldn’t, dwell on things that might have been, because no one knows what, “might have been.” You just do the best you can. You make decisions based on the information you have and the circumstances at the time.
And, almost every time I’m interviewed by a reporter, they say something about how “brave” I am. I find this statement embarrassing. The first time I heard it I didn’t know how to respond. It took me by surprise. Now I tell them, as politely as possible, that bravery has nothing to do with it. Bravery is when a person consciously puts their own life in danger to save or protect someone else. A person who happens to have a disability has not made a conscious effort to be disabled. It just happened. They still have the desire to live as full a life as possible. Just like everybody else. You don’t have to be brave to do this.
Over the past several years I’ve received a few letters from polio survivors who are angry. They feel that they were encouraged, even pushed, to go out and make an active life. They feel this is why they are having trouble now. While I certainly sympathize with them, I don’t agree with this outlook. I’m not sure I would have done things much differently even if I’d known about polio’s late effects. I’m a richer person for the people I’ve met and the things I’ve d
 The FDR Bond: How a Little Girl’s Friendship with America’s Most Famous Polio Patient Changed Her Forever
The FDR Bond: How a Little Girl’s Friendship with America’s Most Famous Polio Patient Changed Her Forever
Anne K. Gross, PhD
On the evening of November 3, 1928, three year old Carol Rosenstiel, her braces hidden under her pant trousers, her wooden crutches digging into her underarms, stood on the platform of Grand Central Terminal in New York City, a huge suitcase by her side. Her mother, Evelyn, holding her three month old son, bent down, straightened the collar on her daughter’s coat, and kissed her good-bye. Her father, Iz, gathered Carol into his arms and held her tightly. Crying, Carol clung to Iz as he handed her over to her Aunt Mary, who had volunteered to accompany her, and the two boarded the train. Their destination: Warm Springs, Georgia, home to the nationally renowned polio treatment center founded by Franklin D. Roosevelt.
Carol was my mother, who contracted polio in 1927 at the age of two, leaving her permanently paralyzed from the waist down. Although Warm Springs had served as a polio rehabilitation center for less than two years at the time of Carol’s visit, its history of healing went back for decades. The first inhabitants were Native Americans, who believed a great spirit lived in the earth, stoking the fires that warmed the springs and healed their battle wounds.
Most people who came to Warm Springs had nothing but fond memories: the feeling of freedom that came from swimming in the warm water pools, the sense of warmth and acceptance for who they were, and the famous Thanksgiving dinners, which FDR graced with his presence every year. But for Carol, her most cherished memories were of her special friendship with FDR, who helped shape her personality and remained a source of inspiration to her throughout her life.
Around the time Aunt Mary and my mother arrived at Warm Springs, Roosevelt won the governorship of New York. A few days later, on November 8, he traveled to Georgia where nearly a thousand townspeople greeted him at the train depot. As his train pulled into the station, he stood on the platform, both arms clenching the railings, as a sea of onlookers proudly welcomed him to his home away from home. Although his visits always engendered excitement, as the newly elected governor, Roosevelt embodied the notion that a disability is an obstacle than can be overcome, fueling the optimism that engulfed Warm Springs.
Carol met FDR in the pools a few days later. She recounted their meeting, handed down as family legend by Aunt Mary, in a series of journals she wrote in the decade before her death in 1985:
Our exercise tables were next to each other and, being the new girl in town, he greeted me with a warm hello and asked my name. I responded by saying “Carol” adding “What’s your name?” To which he answered “Uncle Frank.”
From that first encounter in the pool, Carol was immediately drawn to FDR’s infectious cheerfulness, as he greeted all of the patients with genuine care and interest. Yet what struck her most was here was a man who seemed to not feel a hint of self-consciousness about his impairment. As a result she found her own spirits were lifted.
Carol’s interaction with FDR that day was life-changing, as it stood in stark contrast to how she’d been treated back home. In the 1920s, society viewed polio as a shameful thing, and her parents, who knew of no one else who was stricken with the virus, felt ashamed and deficient as a result of having a daughter who couldn’t walk. Devastated by the thought of raising a disabled child at a time when society viewed people with disabilities as outcasts, Evelyn spent days on end secluded in her room, leaving the care of her daughter to hired help. Thus, at an early age, Carol learned that others retreated in the face of her disability, and soon she began to believe, like her mother, that she was somehow flawed and deficient as a result.
Circumstances were such that Aunt Mary and Carol were renting a cottage across the road from FDR, and soon Aunt Mary began spending her evenings playing cards with the governor-elect and his social secretary Missy LeHand. Carol often spent time at his cabin at the start of the evening, and noticed how FDR, never short of words, drew others in around him. Family lore has it that Roosevelt became quite fond of Carol, probably getting to know her better than most of the children at the center because of the proximity of their cottages.
Once, when a push boy helped Carol into the recreational pool, FDR, who was sitting against the side of the pool, greeted her in his usual “Who have we got here” as he lifted Carol up onto his knees and enclosed her in his arms. As other patients gathered around, FDR peppered them with questions, and engaged them by throwing balls and playing other games. As he ventured from the side of the pool, a swarm of children, including Carol, followed, climbing up on him, pushing him under water, all the while laughing with delight. Later that afternoon, after talking to local farmers in the area, FDR stopped in town to buy ice cream for Carol and all the other children, who rushed in their wheelchairs and braces to greet him as his hand controlled car climbed its way up to the Meriwether Inn, the central meeting place at the center.
FDR’s fondness for Carol was evident at a subsequent swim meet, which Carol later recounted in her journal:
I was pitted against a considerably bigger and older girl … and although I didn’t stand much of a chance of winning I acquitted myself nobly, due no doubt in great part to the fact that Franklin D. Roosevelt cheered me on loudly and lustily through the race. He filled the air with such exhortations as “Come on, Carol. You can do it. Keep on trying. Come on – I know you can do it – try harder. Good girl. You’re getting there.”
As their friendship continued to grow, Carol’s feelings of ease that she felt so keenly after their first encounter blossomed as well. She soon began to believe that the power resided in her to ease the awkwardness of others, most importantly of her parents, and gain the acceptance she most needed, by hiding her own self-consciousness around her disability. Like FDR, she learned to conceal all feelings related to her disability, never once speaking about the emotional and physical challenges she faced, not even to those she felt closest to. And like FDR, she adopted a very gregarious demeanor, deflecting curiosity about her disability by focusing on the needs and wishes of others.
Although both Carol and FDR paid a high price for appearing as if their impairment was nothing more than a minor impediment – including bouts of depression and a lack of intimacy with those around them – it helped them both to be accepted in society at a time when most people with polio rarely ventured outside of their homes.
Fortunately, FDR not only provided a model for how to ease the emotional side of having a disability but also the physical. Practicing his walking on the grounds of the rehabilitation center, Carol noticed how he always walked alongside somebody else, holding on to his or her arm with one hand and carrying a cane with the other, thereby giving the appearance of only slight impairment. With his legs held in place by his braces, he shifted the weight of his body onto his arms and slowly hitched each leg up and forward, smiling broadly while keeping his head up. Outside of Warm Springs, most Americans weren’t aware that he was totally paralyzed in his legs.
This “normalization” philosophy underlined the walking program all patients underwent each afternoon. As elucidated by the head physiotherapist at Warm Springs in a 1932 article in the treatment center’s newsletter, The Polio Chronicle, patients were taught to make “walking smooth, steady and inconspicuous . . . by moving quietly and steadily without needless body, leg or arm motions which would attract attention to the disability.”
Although this was no doubt a tiring and burdensome way to walk, - one that would unknowingly come back to haunt patients years later in the form of post-polio symptoms - seeing FDR made Carol realize that the rewards were worth it. For not only was FDR totally accepted into society, but he was able to achieve the unimaginable. With the memory of FDR’s cheering her on at the swim meet, Carol believed that she too could go on to accomplish great things, and it was here at Warm Springs that her fiercely motivated need to achieve was born. She became a concert musician who performed at Carnegie Hall and recorded with Igor Stravinsky.
In December 1928, FDR left for New York to resume his political career. When Carol kissed her friend goodbye, he told her “I hope to see you again soon at Warm Springs.” Months later, after Carol wrote him a letter, he sent her a letter as well as a photo of himself with the inscription “For my little friend Carol Greenfeld from Franklin D. Roosevelt, Warm Springs 1929,” which served as a testament to their strong friendship.
Carol returned to the rehabilitation center in December 1929, where she stayed for 5 months. Two weeks before she left, FDR came to Warm Springs for a monthlong stay. She eagerly anticipated seeing her old friend, asking Aunt Mary every day when he would come. On a bright sunny afternoon, the two of them joined the flock of patients in front of the Meriwether Inn, awaiting his arrival.
When FDR pulled up – behind the wheel of his Plymouth roaster, a long convertible with the top down – Carol and Aunt Mary rushed to greet him.
“Why look who’s here,” said FDR. “If it isn’t my little friend Carol.”
“Hi, Uncle Frank,” Carol said.
“He's the governor of New York” Mary said. “Call him ‘governor’!”
“Are you still going to play with us in the pool?” Carol asked.
“Of course!” FDR said. “You think I’d come all this way and not play in the pool?” And then he gave one of his trademark laughs – full throated, with his head tilted back. Carol giggled as he exited the car, trailed by other patients. These would be their last days together, as he was not at the center during her two subsequent visits as a child.
Decades later, Carol summed up her special feelings toward FDR in the following journal entry:
Roosevelt was my hero, as indeed he was to all children (and undoubtedly adults as well) who were crippled. The world will not easily forget the special tilt of his chin and all the resolve, courage and determination that made it so unforgettable. That tilt, I believe, had a very special meaning to those of us who shared his personal fate of living with substantial physical impairment, determined to meet the considerable challenge of living our lives fully and well, despite our physical limitations. . . . He was the human embodiment of the Indians’ legendary spirit who lived in the ground stoking the fires to keep the water warm, in order to heal bodies and restore spirits.
Their relationship, however short, impacted Carol throughout her life. Although while I was growing up my mother never uttered a single word to me about her disability, she proudly displayed the photo and letter from FDR in her music room, where it continued to serve as a source of inspiration for her. And in the last months of her life, as she battled cancer, she wrote of FDR in her journals, saying “I need his courage now. I feel strong being ‘one’ with him.”
When I think about my mother – her gregarious personality, her ability to put others at ease by never mentioning her disability, and her ability to draw other people to her – I think of our former president, who had such a lasting influence on a little girl.
Anne K. Gross, PhD, is the author of The Polio Journals: Lessons from My Mother. To learn more about her and her book, visit www.thepoliojournals.com.
Nutrition and Post-Polio
Lauro S. Halstead, MD
This is the story of my personal journey to learn more about nutrition. The path I followed and what I discovered along the way are specific to my body, my nutritional needs and my disability. Some of the principles I learned may apply to others, but the particulars relate only to me. I would no more recommend you follow my specific diet than I would urge you to take someone else's medication. If you want to change your eating habits, please do it under the guidance of a licensed nutritionist. That's what I did.
As it turned out, the nutritionist I worked with had a special interest in chronic disease, although she was unfamiliar with post-polio syndrome. Before going to her, I held what I considered was a traditional but "enlightened" view of nutrition. In other words, I was eating the kind of diet typically recommended in the medical literature and by the experts for a 61-year-old male with my medical history. What I quickly discovered is that "enlightened" is not always smart.
When I was in residency training many years ago, I attended a lecture by an eminent nutritionist who said males should restrict their intake of "visible" eggs to one or two a month; so I reduced mine to maybe half a dozen a year. A short time later, I heard another well-known nutritionist say he was starting his newborn son on 2% milk; I switched that night from whole milk (3%) to low fat (2%), and over the years limited my intake to what I used with cereal.
Then there was the issue of girth control. In the interest of watching my weight, I tried to avoid snacks and sweets, except on special occasions. Fortunately, I don't have a very sweet tooth, so this adjustment was not all that difficult.
And so it went. Over the years, I cut out greasy foods, then lightly fried foods, and finally even lean, red meat. By the time I saw the nutritionist for my first appointment in February 1996, my diet consisted, more or less, of the following:
- For breakfast, one to two large glasses of orange juice, a bowl of raisin bran with milk and one banana;
- For lunch, a large tossed salad with low calorie dressing, a half-pint of lowfat yogurt and fresh fruit; and
- For supper, typically fish or chicken (with occasional red meat), vegetables, potato or pasta, and a salad.
- I also drank a soft drink midmorning and mid-afternoon most days and had a nightcap at bedtime, most evenings.
Sounds pretty healthy, right? That's what I thought. too, especially when I considered that my cholesterol was normal, my weight was essentially the same as when I graduated from college, and people in the cafeteria line never tired of saying, "Wow, that's a healthy lunch!"
Well, my nutritionist did not agree. When I returned after the first week with a diary of everything I had eaten and the amounts, her comment was, "This is incredible," and she didn't mean it as a compliment.
As it turned out, she thought almost everything I was doing was wrong. The bananas and orange juice were 'empty' calories, the soft drinks were a sugar fix, and my lunch was skimpy at best. In short, I was on a starvation diet, in her opinion, which she calculated at 1300-1500 calories per day.
Well, if that were true, I asked, why wasn't I losing weight? Her explanation was that the body makes certain metabolic adjustments to accommodate different caloric intakes.
But it wasn't the caloric intake that bothered her so much. My biggest sin was the small amount of protein I was eating (about 5-6 ounces per day). "No wonder you're tired and weak. Anybody would be on that diet," she said. I, of course, thought instantly to myself, "Is this the cause of post-polio syndrome? Are we all just eating the wrong diet?"
The short answer is "no." But it is clear that a sensible diet can make you feel much better, as I was to find out fairly soon.
The main goals of my new nutritional plan were to increase the amount of protein, increase the number of calories, avoid the empty calories of orange juice and soft drinks, and finally, cut back on that nightcap.
While all of this was going on, I spent a fair amount of time at the library reviewing what's known about protein metabolism and what would be particularly relevant for polio survivors. Here's some of what I learned.
First, proteins are in all human cells. In fact, they form the basic building blocks for each cell, its metabolism, and life itself.
Second, proteins are made from amino acids, and new proteins are being made (synthesized) and broken down (degraded) each day. This protein turnover applies to muscle cells, as well, which are constantly synthesizing new protein every day. Some of this new protein comes from what we eat and some comes from "re-built" protein using amino acids already in the body.
The third thing I learned, and most important for persons with post-polio syndrome, the largest "consumer" of protein in the body is muscle.
All of this means that for the muscles to have a fighting chance to maintain or increase their strength, there has to be a generous amount of protein in the diet. We are not carnivores by chance.
Knowing this, I changed my views on meat and other protein in a jiffy. At the same time, I relaxed my attitude about calories, as well. In summary, I experienced a "nutritional makeover."
It has been almost a full year since my dietary epiphany. I now eat lean meat regularly, along with nuts, fish, eggs, oatmeal and anything else with protein. I do not eat fruit for snacks as much, and most days, instead of a soft drink, I drink a home brew fortified with a protein supplement.
The results? My daily intake of protein has more than doubled to at least 12 ounces per day and my total calories are now somewhere between 1800-2000 per day. My weight is essentially unchanged. The best part is that my "good" arm, which used to be tired all the time, feels stronger, gets less fatigued at the end of the day, and seems to recover faster when it gets overworked.
Is this a "cure-all?" Absolutely not. I estimate my improvement in the 2-5% range, but it hasn't impacted all of my symptoms. I still get intense fatigue in the afternoon. My tank of gas is totally depleted by the end of the week. I'm still searching for new ways to pace myself to conserve what energy I have. Is my new diet healthier living through healthier eating? I believe so. Will it work for others? I don't know. What I have learned for sure, is that sensible eating under the guidance of an experienced nutritionist, is good advice for everyone.
2011 Update
I haven't seen a dietitian in years but have intentionally lost 12-15 pounds in the past six months because of a positive pre-diabetic blood test which scared me but is now back to normal.
Lauro S. Halstead, MD, National Rehabilitation Hospital, Washington, DC
Post-Polio Health (ISSN 1066-5331), Vol. 14, No. 1, Winter 1998, © Post-Polio Health International
Acute polio and its evolution: reminiscences of a 'polio fellow'
Ernest W. Johnson, MD
Returning from 34 months in the southeast Pacific as a GI to my home in Akron, Ohio, I was entitled to four calendar years of a university education funded by the GI bill. I enrolled at The Ohio State University (OSU) and while rooming with a high school friend who was completing his last year of medical school, was given advice-- after joining him on several clinical rotations--to finish the pre-med requirements and use up the educational entitlement in medical school. I did!
As a fourth-year medical student, I was looking ahead to a residency choice, considering anesthesia, pediatrics, physical medicine and rehabilitation, radiology and psychiatry. It seemed logical to defer the final choice until I had experienced these rotations during my internship at Philadelphia General Hospital. My post-MD hospital year began with obstetrics and gynecology, followed by orthopedics, ENT, endocrinology and, by the time I needed to make a selection, I was still confused, so I flipped a coin and it came up psychiatry. I applied for and was accepted in a program at Indiana Medical School. My choice seemed appropriate until my rotation on psychiatry in December. It was a disaster!
As soon as I reported to the service, I was directed to an isolated, high-security room with a locked door, solid except for a small grill. When the door slammed shut behind me, I was imprisoned with a hypomanic patient who was manacled to the bed. Two hours later, I was able to attract the attention of an orderly and be released. I called Indiana and cancelled the residency, too late to apply for another.
A Paralyzing Fear.jpg)
Kathleen A. Navarre
My reaction to the film “A Paralyzing Fear” ran the gamut from objective film critic to the very personal reliving of a long repressed event that seemed to happen to someone else, or in another lifetime, but also clearly happened to me. The event, polio at the age of six in 1952, is at once an intimately personal experience, and at the same time a unifying event that binds all polio survivors by a shared experience. We are all unique individuals as polio survivors, yet one moment in time unites us - the moment the polio virus changed our bodies and therefore our lives.
Regarding my personal reaction, there were some flashbulb memories, the kind of memory that is like a picture, as if the instance remembered was not in the past but a present experience with vivid details long lost in the past. There were the hot packs, too hot for the nurses to touch so they handled them with tongs, the confining heat when first wrapped and then the prickly, damp wool as they cooled off. The haunting rhythm of the iron lung, and my hair being tugged by the rubber neck band as I was pulled in and out of it several times a day. For me, at the age of six, the hair being pulled was the biggest trauma of the day. How little I knew of the future struggle to come, with each year a new challenge, some successes, some failures, but all in all, a very long road ahead.
The one personal and profound insight I had while watching the film was of polio’s effect on my family and on the whole community of my small city. I showed a preview of the film to a support group that I chair. My eight year-old, red-haired, niece was with me for the meeting. At one point I looked over at her, as she was intently watching the film, and was struck by the realization that my parents had to see their red-haired little girl being put in the iron lung and then they had to leave the hospital to go home and raise four other children who were as confused and bewildered as I was by the events surrounding that late summer in 1952. As I looked at my niece, I wondered how I could possibly handle her being paralyzed and further how I could cope with the sad faces that waited at home. Life was changed for all of my family and I deeply respect their ability to handle this overwhelming illness with love and caring.
At the community level, polio as an epidemic has some unique features from other paralyzing illnesses. It was not an individualized event in the epidemic years; it was a public event that brought fear, compassion, and prejudice all at once. In my city of 40,000 to 50,000, it was posted in the daily paper who was hospitalized with polio that week. As the film showed, siblings suffered from being banished from friends, not out of hatred, but out of fear. However, as a child, it does not matter why you are ostracized; you just feel the hurt and go away. In the 1950s there was not the support group concept that would have helped siblings, family and survivors cope with the emotional confusion that was nearly as crippling as the physical disease.
My personal reaction to the film was somewhat like the Vietnam veteran’s reaction to the film “Saving Private Ryan.” One veteran’s reaction was summarized in a quote from “Life Magazine.” He said, “It brought back stuff that I’d never remembered, stuff that happened that I’d brushed out of my mind. It brought it back like a flash, like I was there.” For me, the viewing of the film “A Paralyzing Fear” was painful in parts and helpful in parts. As each individual shared their story, I felt less alone in my struggles, and I hope it is healing in the long run as buried pain can never heal.
Now for the more objective critic’s corner: The people who watched the film who had little prior knowledge of polio’s history, e.g., Warm Springs, Roosevelt’s “Magnificent Deception,” the “Mothers’ March of Dimes,” the vaccine controversy between doctors Salk and Sabin, found the film interesting for a documentary and enlightening. I also found the presentation well done and the narration excellent. The overly dramatic pitch that Hollywood took certainly added to the “poor crippled poster child” image most of us have been fighting all of our lives. It was the approach of the 1950s, and the stereotypes it created live on. I would have liked the film to comment on this issue, but it was an historical documentary, and in that narrow definition, did its job well.
The problem I most take issue with in this documentary regards the ending of the film. As an historical document, the film ends as if the story of polio is only an historical one. As all polio survivors and their families and friends know, just as the polio vaccine has ended one chapter of the history of polio, post-polio syndrome has opened another chapter. The end of this new chapter has yet to be written. Without public knowledge and support, the final chapter is in jeopardy of a less than optimal ending. It is my hope that the film, “A Paralyzing Fear” is a catalyst for bringing new interest, knowledge, research and support for the final chapter.
December, 1998
We Are Still Here
Sunny Roller
As we celebrate the stunning success of the polio vaccine today, I am honored to help commemorate the anniversary by sharing a very personal perspective with you.
Fifty-three years ago, when I was four years old, I almost died from polio. During the acute phase, I could only move one finger. The rest of me was completely paralyzed. Back in the 1950s that disease was certainly spectacular. It struck. It killed. Or it left its permanent trademark on so many of us. Polio left me using two leg braces, a pair of crutches and a back brace.
My struggles when growing up with a disability were certainly continuous. Having to learn to walk all over again, grueling physical therapy, five orthopedic surgeries, and trying so hard to be like all the other kids at school who didn’t use braces and crutches. I knew down deep when my mother gazed at my fourth grade class photo one day, with me conspicuously leaning on my little wooden crutches in the midst of my non-disabled school mates, and said, “you always add such great visual interest to your school picture,” that although not everyone would lovingly accept me with my obvious physical disability the way she did, there was love and support all around me.
Back in the 1950s, she taught me that my attitude about polio was much more important than its physical effects on me. The power of self-determination and social support far out-weighed the power of disability. In fact, we as polio survivors must gratefully celebrate today the astounding amount of social support we received from a fully energized 1950s American community that wanted to save our lives, help us breathe and walk again and succeed in life in unprecedented ways.
Because rehabilitation and eradication efforts were so effective, for thirty years polio survivors blended into society. Polio was so horrible that nobody anywhere in our nation really wanted to think about it anymore, especially those of us who had it. I went to school and started a professional career. The disease was gone, and collectively those of us who had polio were also gone from the national consciousness—almost like medical dinosaurs, fading phantoms of a past era. Everybody waved good-bye to the phantoms as we all went on with life.
But then 22 years ago, when I was 35-years old, once again spectacular polio returned to leave an unwelcome trademark. Debilitating new pain, weakness and fatigue forced me into a whole new series of health care system expeditions. After seeing five different doctors it was concluded here at the University of Michigan Post-Polio Clinic that I had what is now known as the post-polio syndrome. These post-polio symptoms affect half a million polio survivors today in the U.S. alone and confirm that polio creates a progressive condition.
Now I need to use a wheelchair more often. The fear, alarm, sadness and rage I felt at having to fight polio once again are characteristic emotions shared by polio survivors across the country as they too have faced greater disability after 30 years of physical stability. We felt betrayed by childhood physicians who unknowingly told us that not much would change as we grew into our late life years. So we all had to quickly adapt to these unexpected new issues—health care providers, policy makers, medical researchers, polio survivors, their families and friends. And we continue to do so today.
The World Health Organization estimates there are up to 20,000,000 survivors of poliomyelitis in the world right now. We are the second largest disability group in our country next to those who have had a stroke. Because of our history and our large numbers the struggles we have encountered with our physical losses have paved the way for a variety of scientific and social advances.
The medical specialty of physical medicine and rehabilitation (PM&R) started largely because of us fifty years ago. Thousands of children with polio needed rehabilitation in the 1950s. Today PM&R provides critical health care services to large numbers of children and adults recovering from devastating injures and diseases.
In the 1960s the disability rights and independent living movement leading to the passage of the Americans with Disabilities Act started at the instigation of several polio survivors including Ed Roberts and Judy Heumann. They knew our society could do better at addressing the environmental and attitudinal barriers toward disability that were truly handicapping a significant portion of our population, in fact, when you think about it, all of our population. They taught me that not only was my attitude important, but breaking down the external barriers in our communities is absolutely imperative.
In the 1980s the vigorous grassroots movement to address the disabling late effects of polio was energized by thousands of polio survivors in partnership with their health care professionals.
Out of this sociopolitical movement, emerged the now twenty-five year old organization for polio survivors and their health care professionals called Post-Polio Health International. Groups like PHI have promoted networking, advocacy, education and new scientific research that have stimulated the way we think about neuromuscular disease. The risk factors for what are now known as polio’s secondary conditions have been identified and are being addressed for the first time in public health arenas because we were the first to desperately report these issues to our physicians en masse. Because of this, new medical management techniques have been adopted to prudently help those who are facing progressive disability or fast-track aging from a variety of neuromuscular impairments such as spinal cord injury, cerebral palsy or spina bifida. This post-polio movement will help many people who have similar disabilities in generations to come.
Important Disability Studies programs at American academic institutions have been started by polio survivors like Irv Zola in Boston and Carol Gill in Chicago. These programs enlarge and honor the disability paradigm to view people with a wide range of disabilities not as objects but as ingenious producers of knowledge whose common history has generated a wide and rich variety of art, music, literature, and science that happens to be infused with the experience of disability.
As we celebrate the annihilation of the disease called polio today, we recognize that there is much left to be done. Polio survivors still have important needs for knowledgeable health care providers in many fields of medicine who are thoroughly educated about polio’s late effects. With the large generation of aging polio survivors at the forefront, public policy makers need to address many other instrumental needs of polio survivors. These include the new early retirement requirements of adults who will be aging with a lifelong disability, which will also help so many baby boomers who are aging into a disability. We cannot let our social security system collapse. Medicare and Medicaid need to get stronger. Issues of health insurance coverage for personal assistance, health and wellness activities, long-term health care and assistive technologies are important to address. Housing and transportation opportunities need to become more affordable and accessible. These are all public health issues that need to be addressed in public policy arenas and the private sector through organizations like March of Dimes and Rotary International.
Let us celebrate the fact that huge numbers of us who have been living with the effects of polio for over fifty years have quietly figured out how to thrive and make substantial social and political contributions in a non-disabled world. Most of us are not famous, but some of us are, like Itzak Perlman, Alan Alda, and Joni Mitchell. We also recall the luminosity of Franklin D. Roosevelt.
Getting polio is mostly a thing of the past, thank goodness, but we who had polio are alive and have been here all this time! We are with you! Now that our average age is about 65 years, as we look back, we know that we have experienced the issues and challenges of physical disability with a longevity and fullness never before known in the history of mankind. Before it’s too late, we need to share our wisdom about living and loving with a life-long disability with the world. I believe that we as polio survivors have within us, both individually and collectively, a wealth of knowledge and insight that can help others grow and flourish. We still have so much to contribute, which, thanks to the ongoing compassion and concern of all of us…we will do.
Sunny Roller, MA, Presentation at the Salk Celebration, University of Michigan, April 12, 2005.
The Miracle of the Singing Bunny
Sunny Roller
Her bright blue-eyed pre-kindergarten daughter lie flaccid in a hospital bed, almost completely paralyzed from polio. Now 60 years ago, that horrifying summer polio epidemic had swooped this young family into its vile clutches, never to fully let go during their generation. Devastated, Marj, her husband, Art, and their toddling one-year old son, Scotty somehow got a ride back and forth to the urban acute care hospital every day to see Sunny. It was 1952 and the couple didn’t even own their first car yet.
Throughout their frightening earliest bedside visits, they knew death loomed all around. Children with polio were dying in the beds nearby. Would their firstborn little girl live or would she die with the others?
After what seemed an eternity of days, an attentive young nurse approached them smiling, “I have good news. We’re out of the woods! Sunny will be okay. We don’t know how much strength she will regain though. The doctors say she will need about nine months of rehabilitation now, likely followed by several orthopedic surgeries and years of physical therapy. But she has survived!”
So now it began—this young family’s search for the strength to stay endlessly hard working, encouraged and optimistic. Marj lovingly asked Sunny that afternoon, “What would you like me to bring you tomorrow, Sunny? What would make you feel better?” Sunny searched her imagination. “A singing bunny,” she softly whispered.
“Yes,” Marj thought. “Perfect. A cuddly and cheerful bed-friend with a music box inside to hold close and sing to her in this humorless hospital.” “Okay Honey. I will bring you a singing bunny…”
Do you believe in miracles? I do. I recently read that nearly 80% of Americans do too. I have seen miracles, felt the presence of encouraging and comforting angels and have encountered many spiritual inspirations. They are often what helped me get through my tough lifelong encounters with polio. With this in mind, let’s get back to the story about a miracle that happened to my mother long ago in 1952 …
Marj left the hospital that afternoon determined to make Sunny a singing bunny. She found a stuffed toy rabbit at home in a box of playthings. She figured out that she could snip a slit in the fabric, dig out a little filling, and then find a small music box to sew into the bunny. But in searching through all the toys, she found no music box anywhere in the house. So, determined to get to the shops before they closed, she swooped Scotty up, lowered him into his baby stroller and bustled half a mile downtown to buy a music box. Sunny must have a singing bunny! But after searching the shelves and inquiring in every promising shop downtown, she was left bereft. Every single merchant told her, “Sorry, we have none.”
What could she do now? A musical stuffed animal was her fragile little girl’s lone request. And this mama knew that right now, a singing bunny could be the one special buddy Sunny needed to keep her company through the grueling months of stinky hot packs, painstaking physical therapy and learning to walk all over again with orthopedic braces and crutches.
Bewildered, Marj plodded along the sidewalk toward home, mindlessly steering her son straight ahead in the baby stroller. Suddenly a sparkle in the grass caught her glimpse. As her eyes focused downward to the shiny object, she couldn’t believe what she saw. It was a little music box that someone must have been dropped or thrown away. Amazed and delighted, she snatched it up and wound it up. Dingling a tune, it worked! Racing home, Marj washed the newfound treasure off and carefully stitched it into the awaiting stuffed rabbit. Together Marj and Art delivered the new singing bunny to Sunny the next day. And that bunny stayed close and served its purpose as part of the family for years to come. Actually he’s still around somewhere.
I’m so thankful that Mom shared this story with me before she died. She taught me that there are unexplainable events in our lives that help us get through. And just as Mom shared her account with me, I believe that we may very seriously want to consider sharing our life experiences with the children and grandchildren in our lives. Who we are and what we have experienced in life can offer young people a sense of their genetic heritage: describing where they came from; endorsing what they can still become.
Recording our life experiences might be a wonderful project to do in our support groups. Together we can begin to encourage one another to document our personal stories either in writing, on audiotape or DVD. Each person might write a comprehensive memoir or just one or two short stories. The support group could invite a guest professor from a local college to help members learn about how to write effective memoirs or successfully record oral histories. The group also might want to engage a local media specialist to help certain members create quality DVD recordings.
Support group members could choose to compose short autobiographical stories that teach life lessons or illustrate personal values. We could document individual experiences about overcoming the odds or taking risks that either paid off or failed. We could tell about the role of people we encountered throughout life that either helped us succeed or who were desperately difficult and discouraging. We could write at home, and then bring the stories to group meetings to share--even engaging each other to constructively critique the writings for diction and syntax. Another option might be to find a child, grandchild or student who needs “service-learning project” credit to record our life stories. We might even find a budding journalist like the lead character in this year’s movie, The Help, to listen and write it all down for us. Whatever works!
As polio survivors, we have a rich legacy to leave. We have experienced life from a unique and important perspective. Believe it or not, the “kids” in our lives want to hear from us directly now more than ever. And frankly, we’d better do it fast.
What People with Disabilities Hope for from Other People
Fr. Robert J. Ronald, SJ, Taiwan
Please don't notice only our disabilities. They are the first thing that you see, but they are not the most important thing there is to know about us. We hope that when you see us you will say to yourself, "Here's somebody like me, who may have some abilities, interests or aspirations similar to mine. I wonder if there is anything I can do to help keep the disability from standing in the way of their realizations."
Please don't exaggerate our disabilities or suppose we're all alike. People have shouted at me as though I were also deaf and talked to me like a child as though I had never grown up. Or, because I'm in a wheelchair like their grandfather who just died, they think they know all about me. We hope that you will think when you see us, "Here is somebody who has something interesting to say if I will stop and listen. And something interesting to do if I'll give him or her the chance."
Please don't think of us only as people who cannot do things. We are just people who cannot do some things the regular way. I cannot walk from here to there, but with a good wheelchair I can still go from here to there. A blind person cannot see the words in a book, but with Braille can read the book. We hope that when you see us you will not say to yourself, "How sad that this person can't do the things I like to do or go the places I like to go or work where I do." We hope you will think instead, "Too bad about the limitations, but no matter. What kind of training or special equipment or ramps are needed, so that he or she can also do the things I like to do or go the places I like to go or work where I work?"
Please don't deny our disabilities or treat them lightly. They are something very real to us with serious, permanent effects on our lives. We hope that you too will acknowledge the difficulties we face and pitch in to help us remove the barriers and problems. If we are discouraged, encourage us not by distracting us to think of something else but by showing us practical ways of coping.
Please feel with us our grief and anger and frustration. Often the best way of handling such feelings is to get them out in the open where they can dissipate. Don't take as personal insult or rejection what we might say or do in your presence on such occasions. Instead of just telling us to shut up or to cool it, show us you understand and empathize with our point of view. But if we persist in bemoaning our losses, make your encouragement practical. Point out to us all the things we can do. Help us find a goal for our lives that appeals to us and which we can attain even with our disabilities. Then as our friend show us how to reach that goal.
Please don't think that we are all inferior and depressed and would rather stay with our own kind. Sometimes this is true, but if we manifest fear or hesitation or distrust or believe that we cannot do a lot of things, it is usually the result of bitter experience. Some people stare at us, avoid us, laugh at us, pity us, overprotect us. Everywhere we meet barriers. We have learned inferiority from being relegated to inferior status. What we hope for from you, therefore, is positive regard and feedback. We will more readily learn to value ourselves the more we experience you valuing us, accepting us as friends and associates, and providing us opportunities for participation, self-expression, growing and giving.
Please don't pity us. Disclosing horror or sadness at our situation only makes us feel worse. We need solutions not commiseration. Show us you believe these obstacles can be overcome. Show confidence that we can still lead wonderful, full lives. Don't deny the hard work or the difficulties that lie ahead of us, just help us move forward.
Please don't be afraid to notice our disabilities or ask questions, but do it right. Curiosity is not always bad, since asking each other questions is one of the best ways that friends have of getting to know each other. So look at us, ask all the questions you want, but just don't treat us like animals in a zoo without feelings. It is degrading when people pay all their attention to our wheelchairs, caring nothing about ' When you look and speak, do so in a way that shows respect for us as persons and interest in us as potential friends. And don't forget to give us a chance to know something about you, too.
Please don't make decisions for us or tell us what we should do. What we are and wish to do should not be defined by our disabilities but by the nature of our particular abilities, interests, aptitudes and ambitions. we may need your suggestions and advice for which we will be grateful. We may even need to be cautioned if we want to bite off more than we can chew, but remember, it is the size of my mouth and not yours that determines how much I can chew.
Please offer us help if you see that we need it. Please ask first whether the assistance is wanted; then ask how the help should be given. Do it as inconspicuously as possible. You may want the whole world to see that you are doing your good deed for the day, but we would rather no one noticed that we could not do things for ourselves.
Please be patient with us and fair. We people with disabilities are not perfect, nor always on our best behavior. In this, unfortunately, we are all too normal. Like everyone else, we are sometimes in the dumps and sometimes on cloud nine; sometimes lazy, demanding help we really don't need; sometimes stubborn, refusing even the assistance we do need; sometimes friendly, sometimes hostile; sometimes placid, sometimes angry. We do not ask you to ignore our faults. We should be accountable for our actions like everyone else. But at least show us as much tolerance for our short-comings as you show your other friends and colleagues for theirs.
Please don't tell us how wonderful we are because we smile so bravely or try so hard. In the first place, we already know it, having been told so a million times before. In the second place, this is actually rather discouraging. Here we are just trying to do the ordinary things every one else does all the time and someone gushes over us as if it were something extraordinary. This tells us the person really thinks our disabilities are awful and our capabilities low. Yes, we do have to try harder. Yes, we do deserve credit for the extra efforts we have to make, but we would much rather have you pitch in and help us reach the rest of our goals than just applaud what we have already achieved.
Please don't tell us we are already doing enough or to stop trying so hard. It makes some people uncomfortable to see us struggling with our wheelchairs or assistive devices or they want us to accept our disabled lot quietly, graciously submitting to the status of being served instead of trying to serve. Perhaps some of us have reached the limits of our capabilities or are content to maintain our present positions, but the decision when to stop should be ours, not yours. Many of us still have abilities and inner resources we want to develop and use, even if it is going to be difficult. Disability does not take away our right to pursue the full development of our potentials. Instead of preparing us a comfortable place to rest at the bottom of the stairs, we would rather you help us find a way to get up the stairs to where the action is.
© Post-Polio Health (ISSN 1066-5331), Vol. 4, No. 4, Fall 1988
PPS Pain and Fatigue
Linda Cannon Rowan
When I complain to my doctor about pain or fatigue, he usually tells me that I am not getting enough rest.
I GET SO TIRED OF HEARING THAT I NEED TO REST! BUT I KNOW THAT I MUST!
A day without pain is rare.
I was told when I was first diagnosed not to do anything to cause pain or fatigue because I may cause more damage to my nerves and muscles. But exercise is encouraged…so you have to find the level of activity that is best for you. My physiatrist told me that he loves his PPS patients because “all I have to do is to say, ‘Don’t do that!’ ”
Let’s see…what causes me pain and fatigue? Breathing too much...sitting up too long…holding my head up…chewing bubble gum or holding my mouth open at the dentist…walking, standing, sitting. Any activity that involves using my arms or hands without rest for short periods of time, such as: driving my van with my hand controls, sewing a hem into a skirt or pair of pants, holding up a newspaper or book without it resting on something, drying off after a shower, taking a shower in the first place. Did I say just breathing makes me hurt and causes fatigue? I know I did. That would have been almost unthinkable to me way back when I first heard I had post-polio syndrome. Now I have to use my Bi-PAP at night to do the breathing for me so I can breathe unassisted during the day without pain in my chest.
I think the worst kind of pain associated with post-polio syndrome is what I call the “Polio Flu”. This is usually brought on by long periods of activity when you FEEL “OK” while you are doing it (so you just keep on until the task is complete). I call this “Polio Flu” because the pain is like the worst case of flu you ever had…all of the muscle aches and pains similar to the it but without the respiratory congestion of the real “Flu.” When you finally lie down, a fatigue that overwhelms your whole body just pins you to the bed. It feels like your body must weigh 1000 pounds! You are hurting, but so tired that you can’t move…not even to go get pain medicine or even to cover yourself if you are cold. You may be hungry, but the thought of moving one muscle to get food is just way too much! The pain is in every muscle: legs, arms, body, even your eyeballs hurt to look around the room. At times I have been way too tired to even talk. My Mom used to call our home and sometimes if Terry told her I was resting, she might ask, “Can she TALK?” And she didn’t mean could I talk TO her, she meant was I ABLE to talk!
Over the years, I HAVE learned to pace myself…more out of necessity than anything else. My tolerance for driving my wheelchair van, even with “1/2 Effort Assisted” steering and brakes, has lessened. I can describe it more in miles than anything else. Ten years ago, I could easily drive my mother to one of her doctors near the hospital, which is about 20 miles from my home. We could have a nice lunch, and stop and shop at a couple of stores while we were out that day. Mama walked, and I used my wheelchair. Every stop requires me to transfer from my van’s driver’s seat to my wheelchair.
Starting about five years ago, I couldn’t take her to her appointments anymore. She had to change one of her doctors because we needed one that was closer to us. I can drive to the library, which is seven miles. I can only handle about two stops in a day, one if it is somewhere like Wal-Mart or a doctor where I have to wait. On these days when I am going to be out, my husband either takes me out for supper or calls for a pizza or I have “planned” leftovers, so I won’t have to cook when I get home.
The next day I almost always require total rest. Several years ago I had to stop attending Women’s Bible Studies and mid-week services at my old church which is about nine miles from home. I now belong to a sister church which is only two miles away. I can attend many more things and am not as shut in because of its proximity to my home. But I still have found that it is nearly impossible to get to the morning Women’s Bible Study that starts at 9:15 am.
When I go to church or to a week day Bible Study, I have to get up at least 2 1/2 hours early. I often have to rest after I shower and rest again after I dress. If I have to rush out of the house an hour after I get up, I am “done in” for the day. This is my life. My doctor said that he wishes that more of his patients knew how to pace themselves like I do. Well, if I am doing it WELL, I’d hate to be one of his patients who don’t know “how to pace themselves.” I do what I do out of necessity.
Post-polio has caused many other problems with my nerves, muscles and joints and I hurt somewhere all of the time. My physiatrist told me that I don’t take enough pain medication. We have an on-going feud about this. I feel that pain is an indicator that something is wrong. More pain than “normal” for me and I know that something I did has caused it. I usually know what it was and adjust accordingly. For me, as a general rule of thumb, I need about twice the amount of time to recuperate from something I did to cause pain or fatigue. For example: one week vacation at a resort requires at least two weeks total rest when I return. I “rest up” before I leave home. I rest every afternoon while “on vacation”, but the preparation for the trip, travel and getting settled again when I get home end up doing me in. Lunch out, a little shopping and a movie with my husband driving my van will cause me to have to stay in bed most of the next morning. I will not discuss pain medication here because different things work for different people and no two people are alike.
Making the Most of Time
William Stothers
It all depends on your disability, of course, but most of us probably pay out more money, and most likely more time and energy, to manage our daily routines than non-disabled people.
For example, even with health insurance, I shell out a steady flow of funds for wheelchair repairs, other orthopedic equipment and ventilator supplies.
All those costs are only the beginning. I spend a lot of energy (my tank seems to empty faster these days) and time on my own disability to shore up my independence. For instance, it takes me two to three hours to get up and moving in the morning.
The alarm rings at 6:30 a.m. usually, and I begin my routine. Fortunately, with the assistance of my wife, also a polio person, I am able during this time to drink a cup of coffee, read my local newspaper and listen to NPR. After unhooking my BiPAP machine, I haul myself on to my bedside commode for an extended period – this is essential for me because once I get into my power chair and dress myself only the direst emergency can get me back to bed before nighttime. It’s just too hard to do. Before I retired from a job that required me to be at my desk by 9 a.m., I got up even earlier and was much more focused, urgent and stressed in my routine; nowadays I am more leisurely and gladly spend – and even relish – this time.
We try as much as possible to keep up our house ourselves. Cooking, doing dishes, policing the clutter that inevitably accumulates; all get done even if we spend more time and energy doing these jobs than other people.
Some jobs, though, are beyond us. Changing light bulbs in ceiling lights, batteries in beeping smoke detectors, doing laundry, cleaning the bathroom, cutting the grass are some of the chores for which we have enlisted help.
Sometimes that takes more time (time, again!) than expected. We have eaten dinner by candlelight on several occasions when the bulb blew as the mac and cheese floated in from the kitchen. If only we could time it so that the bulb would go out when we have dinner guests, guests that is, who were able to change the bulb, not always the case in the circles we roll in.
Happily, we have neighbors willing to help take care of many of these often annoying little household crises. And we are able to pay a housekeeper once a week and a garden man twice a month.
But, we have often felt in the past that our neighborly help tasted like charity. People helped us, and we were truly grateful. However, it was a one-way relationship and that bothered us. Over time we have developed an exchange system, largely unstated, that opens the way for us to help our neighbors, too.
We have writing, advocacy, office and computer skills that we have used to help our non-computer using neighbors (yes, there are people like that out there) find information they need.
We have a van that we help car-less neighbors go shopping or to appointments, and rescue friends with disabilities whose wheelchair vans have broken down.
Lately, we have become aware of a movement called “time banking,” wherein people donate an hour or more of time to assist another person, and in return, they can claim an equal amount of time for help from someone else.
Time banks are a kind of intentional community, which can be its own social reward. Time banks can be centered in a local area, or spread more widely if mobility is not a critical issue.
Have you had experience with time banking or other ways of exchanging, saving or stretching time – on the deficit or surplus side?
I would like to hear about it. Let’s share, and we can all get more high quality time and help others as well. That’s time well spent.
Bill Stothers is a long time editor and consultant on media and disability policy. He edited Mainstream, a national advocacy and lifestyle magazine for people with disabilities and major newspapers in Toronto and San Diego. He is a member of the Board of Directors of Post-Polio Health International and currently serves as its Chair.
Response: I was fortunate to regain a good life after contracting polio in 1952 and lived a normal life until 2004. But, post-polio has hit with a vengeance, but still blessed because many are much worse. I had bulbar polio which now has wiped out my ability to be understood. I have lost my balance in my right ear, thus needing a walk or scooter when my legs give out. I have 50% lung capacity, restricted swallowing and vocals. I do most of my eating through a feeding tube. I tell you all this to let you know the level of my need. Still I live alone and can manage my personal needs, but I also pay for help to clean my house and take care of the yard. I also look for fund raisers that donate time for contributions to get special projects done - I can always use the tax right-off. A type of time bank since my ability to give time is very limited.
Your article on time banking intrigued me, not just for disabled needs, but for connections in times of disasters. There are times I feel isolated, especially when not feeling well. My closes family member is 20 minutes away. I do have kind neighbors that have helped out in urgent situations. My property is on a slope and I've twice tipped over my scooter in the yard. I was fortunate that both times a neighbor saw me and came running. This isn't a true time bank, but I always write a nice thank you note with cookies for their help. I don't feel obligated, just grateful.
Also, I carry a sell phone for safety reasons and I have neighbor's phone numbers that have agreed to be of help when I have a need. I don't take advantage of them, but it is a secure feeling to have them available. If I fall, I am not strong enough to get up and they have been there for me a few times.
Donna Bleiler
Learning from Disability
Grace Young
My life changed course when I had polio at age nine, but I was too young to realize it. When a person is disabled in adulthood their whole world is turned upside down pretty quickly. At the age of nine, I only knew that I couldn’t walk, play outside with my friends, or go to school for a year. But what really charted the course for my future was being a patient of a physical therapist, Miss Waddell, who had been trained by Sister Kenny.
Along with the dreaded hot packs five times a day, there was muscle re-education every day. This was the interesting part. Miss Waddell believed in using the correct muscle name as we did each exercise. None of “squeeze this muscle,” rather it was “the anterior tibialis starts here and ends here, now contract your anterior tibialis.” I left that hospital the best muscle-educated ten-year-old you could imagine. The therapy continued with others after I came home, but Miss Waddell definitely set me on my life course.
When it came time for college, choosing a profession was easy. Although I seriously considered both occupational therapy (OT) and physical therapy (PT), OT won out because of my love for crafts. And - of course - what specialty area would I choose besides physical disabilities? Post-polio syndrome (PPS) didn’t rear its head till many years later, so that was one disability that was not in the therapy curriculum. Polio was considered stable: no one knew that the other shoe was just waiting to drop.
Eventually I became weaker and less mobile, and started needing to use a brace and walking aids so I could keep managing my work and home life. Thirty years after graduating from college I was back in school getting a master’s in OT so I could help myself and others cope with what was happening to us. After that one thing led to another and I made PPS a sub-specialty in my work.
My daughters also learned from my disability. They learned to be resourceful, helpful, sensitive and accepting of people different from themselves. Along with the skills of problem-solving, they can determine whether an environment is truly accessible; they are the only able-bodied people whose judgment I can totally trust.
Emotionally, what have I learned? That life is unpredictable, that things happen, that we need to be ready to adapt because life doesn’t always turn out the way we expected. We have to learn to accept help from others for those things that we used to do for ourselves. That we need to be grateful for the help we get and thankful for whatever abilities we still have.
© Grace R. Young, October 2008
Courtesy of Sharon Lark
Facing Reality
Grace Young
My most shocking revelation was that I really did have a disability. That didn’t happen for almost forty years after I had polio. At age 46 I started working at Kaiser and my supervisor asked me, “Grace, do you consider yourself disabled?” It was the height of affirmative-action consciousness and he needed to identify minority members of his department. But the question felt like a slap in the face. Why would he ask that? I thought about it and finally said, “I guess I am.” That wouldn’t be a strange reply if there had been any doubt about it. But I had worn a long leg brace and had used handicapped parking for several years. Yet I never considered myself disabled.
By age 50 I still didn’t use any walking aids (the long leg brace was an “invisible” aid - hidden by long pants). Didn’t even use a cane to get up to the Acropolis in Greece (but had a husband and two daughters pushing and pulling). But after that trip I knew I needed a cane and by the next trip I needed a crutch. Each new layer of equipment made me feel like I had lost something that I could never get back - I could never again pretend to be a “passer.” But the most difficult decision was realizing that I couldn’t continue working unless I used a scooter. The walking, standing, fatigue, increasing weakness - it was all leading to an early retirement that I didn’t want and couldn’t afford.
Here I was an occupational therapist treating people with various physical problems. I had to wonder: a therapist driving a scooter - what would patients think if their therapist looked more disabled than they did? This was going to be a whole different experience but I didn’t have any other options.
With each new piece of equipment, life changed for the better. I had to ask myself why hadn’t I done this before? I am sure that working so hard to fit into an able-bodied world had caused me to go downhill physically much faster that if I had faced the reality that had been staring me in the face for so long. Yes, I had a disability. Yes, I needed equipment. It was the greatest relief to not have to straddle two worlds anymore.
© 2008 Grace R. Young
Courtesy of Sharon Lark
Past and Future
Grace Young
When I had polio at age 9, I was happy to have a wheelchair - any wheelchair - that would allow me the freedom to leave my bedroom. The only model available at that time was all wood with a cane back and wooden wheels. Undoubtedly it’s featured in the Smithsonian now. Large, heavy, clunky - forget taking it outside the house. It was a feat to even move it inside the house. Once I was parked in a room I stayed there until someone came along to push me somewhere else. If an object got dropped, it stayed on the floor until someone came along to pick it up. I did develop a useful talent, though. I became an expert in reading four different books at the same time. The living room, dining room, bedroom, and kitchen--each had a book that I could resume reading if that’s where I happened to land.
Well, I can’t resist reminiscing about times past because it makes me appreciate the life I have now as a disabled person, imperfect as it is. So what would I predict for the future? There are two phenomena that I think bode well for the future of people with disabilities.
The first is the “Graying of America,” a phrase that is very relevant to us. Almost everyone who lives long enough will have mobility problems, as well as difficulties with bathing, toileting, dressing, housing, transportation. There have been many improvements, but we still see bus drivers not trained to use their lifts, unramped streets and buildings, narrow doors, inaccessible toilets, fire hydrants blocking sidewalks, too little crossing time at streetlights and people with attitudes of exclusion. Ruth at Wheelie Catholic describes her situation where the bus driver had not been trained on how to use the bus lift and tie-downs and the other passengers very vocally displayed their displeasure at being delayed. However, the good news is that as a larger percentage of the population gets older, people with disabilities will benefit from improved (and in some cases enforced) accessibility, accommodations, and—especially—attitudes.
The second phenomenon is the result of a war most of us wish had never happened. Starting in the near future, thousands of profoundly wounded service men and women will complete their rehabilitation and enter society with special needs that match or exceed those we have been living with. These wounded warriors may be the impetus that will accelerate the changes that we have been working for. More government and private funding will be earmarked for research into equipment, housing, environmental adaptations, transportation, health care, and other areas to meet those needs. I anticipate that, along with attitude changes toward accommodating people with disabilities, the resulting improvements will trickle down and benefit all of us.
© 2008 Grace R. Young
Courtesy of Sharon Lark